Endoscopic & Minimally Invasive Spine Surgery (M.I.S.S.) Clinic (Center of Excellence)
Services
«The main purpose of the philosophy for the treatment of spine conditions, is to achieve the best possible result for the patient, with the least possible surgical intervention and the least pain».
The Endoscopic & Minimally Invasive Spine Surgery (MISS) Clinic, with the excellent scientific training and extensive experience of Dr. Georgios Vastardis, MD, PhD, in full edoscopic spine surgery and minimally invasive techniques, constitutes a certified Center of Excellence in the field of endoscopic spine surgery, by Elliquence as a Center of Excellence for Full Endoscopic Spine Surgery.
-
Spine conditions
Most of the general population experiences spine-related problems during their lifetime. Traditionally, the surgical treatment of these problems –when it was decided– included major-mutilating surgical techniques, without the application of strict scientific evidence, which often led to a negative result for the patient. The most important spine conditions are:
- Degeneration and dehydration of the intervertebral discs (Degenerative Disc Disease)
- Traumatic intervertebral disc herniation
- Inflammation of discs and vertebrae, such as spondylodiscitis
- Spinal stenosis
- Spinal injuries
- Tumors of the spine and spinal cord
- Spinal deformities, such as scoliosis and kyphosis
- Spinal fractures which are due to low-energy injury or spontaneous subsidence of the vertebral bodies due to osteoporosis or other pathological causes and
- Failed Back Surgery Syndrome
The philosophy of Minimally Invasive Spine Surgery is to minimize the destruction of muscles and other tissues that support the spine, in order to achieve, as much as possible, the patients’ immediate postoperative mobilization and rapid return to their daily habits. This is achieved by applying modern, innovative, minimally invasive suitable techniques that involve the entire , cervical, thoracic and lumbar spine.
-
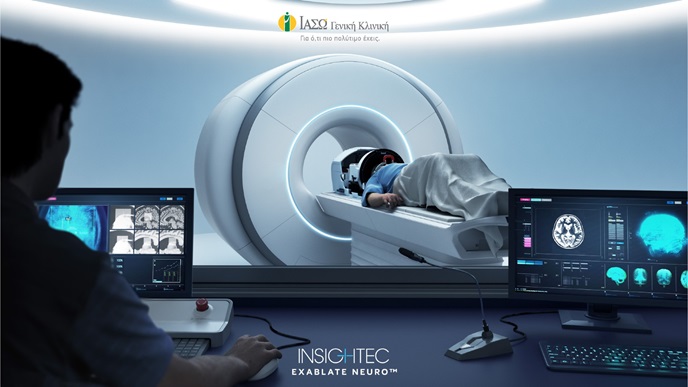
Minimally Invasive & Endoscopic Spine Surgery
Minimally Invasive & Endoscopic Spine Surgery treats the entire spectrum of spine conditions (cervical, thoracic, lumbar and sacral) with contemporary, advanced techniques. These techniques, most of them percutaneous, are performed with small skin incisions (~1cm) and the use of microtechniques under magnification. In this way, bleeding is avoided and the destruction of adjacent tissues is minimized, achieving a perfect surgical result.
Recovery-healing following the operation is quick and postoperative pain is often nonexistent. Patients are able to and do leave the hospital in as little as 24 hours or even on the same day, just a few hours after surgery. They are immediately functional and can return to work in a very short period of time.
-
Applied techniques
Minimally Invasive Spine Surgery includes techniques such as:
- Epidural,
intrathecal infusion (Block), the blocking of the facet joints and injections in the sympathetic nerves.
The aforementioned methods treat chronic or acute pain in the spine and spinal nerves with local injections of substances under fluoroscopic guidance along the length of the spine and under local anesthesia. - The thermal or chemical reduction of the core of the intervertebral disc, (discoplasty) in case of pathological causes.
- Endoscopic
treatment:
- Removal of disc herniation as well as plastic surgery of this annulus fibrosus, in order to minimize postoperative pain and complications.
- Rhizotomy for lower back pain (backache) originating from arthritis or inflammation of the posterior joints of the spine (Facet Joints) by denervation the collateral branches responsible for causing the pain with the help of laser or special diathermy.
- Decompression by fenestration or hemilaminectomy in cases such as central spinal stenosis.
- Foraminoplasty, meaning the opening- widening of the foramina and decompression of the neural structures in lateral-foraminal stenosis.
- Endoscopic spinal fusion.
In the event that more extensive decompression is needed, this can also be performed via special percutaneous dilators through which the decompression is performed micro-invasively, as well as via percutaneous spinal fusion, which means the placement of screws and interbody cages to stabilize the spine without a wide incision.
- Kyphoplasty
The traumatic or spontaneous fractures of the vertebrae are a different chapter of spine conditions. The treatment of stable fractures of the spine which are due to some injury or to an automatic mechanism as a result of strain on the spine and some accompanying pathology such as osteoporosis or other conditions, is carried out with the percutaneous kyphoplasty method. Percutaneous kyphoplasty is a method through which internal realignment and stabilization of fractures is achieved percutaneously, without the need for transfusion, while the patient can stand and walk immediately after the operation, without support. The patient may return home in less than 24 hours, pain-free.
Stable fractures of the spine due to some injury or to an automatic mechanism as a result of strain on the spine and some accompanying pathology such as osteoporosis or other conditions are treated via percutaneous kyphoplasty, meaning the internal realignment and stabilization of the fractures percutaneously, with the intraoperative use of a special fluoroscopy, without the need for transfusion, while the patient can walk without support immediately after the operation.
In the event that the patient needs a wider decompression in the spine for a certain reason, decompression is performed percutaneously, micro-invasively or endoscopically, and the same applies for percutaneous spinal fusion, meaning the placement of screws and interbody cages to stabilize the spine with the intraoperative use of a special fluoroscopic C-arm, and/or with the use of a special O-arm navigation system or Robot guidance, when it is needed.
Many of the aforementioned techniques are performed with local anesthesia. Thus, the patient leaves the hospital usually on the same day, meaning a few hours after the operation, returning to his/her usual activities as soon as possible.
In contrast to the up to now large incisions to treat similar pathology (canal and foraminal stenosis, herniated disk, injuries), the same result or an even better one and with fewer complications is achieved with the above techniques. Minimally invasive surgical techniques are also applied in order to treat spinal deformities such as scoliosis and kyphosis, in adults and children, as well as to treat failed back surgery syndrome (FBSS).
Many of the aforementioned techniques are performed with local anesthesia. Thus, the patient leaves the hospital usually on the same day, meaning a few hours after the operation, with instructions on what to do at home, returning to his/her usual activities as soon as possible.
For the effective treatment of spine conditions, the principles of evidence-based medicine must be strictly applied, meaning the proper treatment of each patient's complaints according to specific, internationally accepted, therapeutic directions, based on new scientific data ("Evidence-Based Medicine”). The step-by-step treatment of spine conditions is of particular importance, based on scientific documentation, from which the success of the respective treatment is evaluated. The main purpose of the philosophy for dealing with spine conditions is to achieve the best possible result for the patient, with the least possible surgical intervention and the least pain.
- Epidural,
intrathecal infusion (Block), the blocking of the facet joints and injections in the sympathetic nerves.
-
Advantages of Endoscopic Surgery for the patient
- Small skin incisions (~1 cm) resulting in the minimization of the destruction of the surrounding tissues
- Avoidance of bleeding
- Local anesthesia in most techniques
- Fast postoperative recovery-healing
- Almost no pain after surgery
- Shorter hospital stay: patients are discharged either a few hours after the operation or the next day
Georgios Vastardis MD, PhD is a Spine Surgeon that completed his two year fellowship at Loyola University, Adventist Hinsdale Hospital and VA Edward’s Hines, Chicago – USA and he is a member of the North America Spine Society, International Society for Minimal Intervention in Spinal Surgery (ISMISS) and Scoliosis Research Society. Dr. Georgios Vastardis, MD, PhD, is among the top internationally ranked instructors for Endoscopic Spine Surgery (International Instructor for Full Endoscopic Spine Surgery).
Dr. Georgios Vastardis was also chosen as Ambassador and International Instructor of Endoscopic Spine Surgery by Elliquence, based in New York, USA. In the context of this distinction, in which doctors from all over the world are selected, he attended the Elliquence Training Institute in New York on Saturday, March 26th, 2022, where he held a Full Endoscopic Spine Comprehensive Course with hands-on training in Endoscopic and Minimally Invasive Surgical Techniques. During the Course, Dr. Vastardis trained young doctors in the latest techniques in a live spine surgery. The same happened in Australia on May of 2022 where he was the first worldwide that was invited to train for the first time in Australia, specialized spine surgeons in full endoscopic spine surgery.









